Long-term care spending set to double or triple by 2050 - OECD
Spending on long-term care in OECD countries is set to double, even triple, by 2050, driven by ageing populations. Governments need to make their long-term care policies more affordable and provide better support for family careers and professionals, according to a new OECD report. This is a very significant report in the context of Ireland's 'Fair Deal' programme providing long-term care for older people does not have sufficient funding.
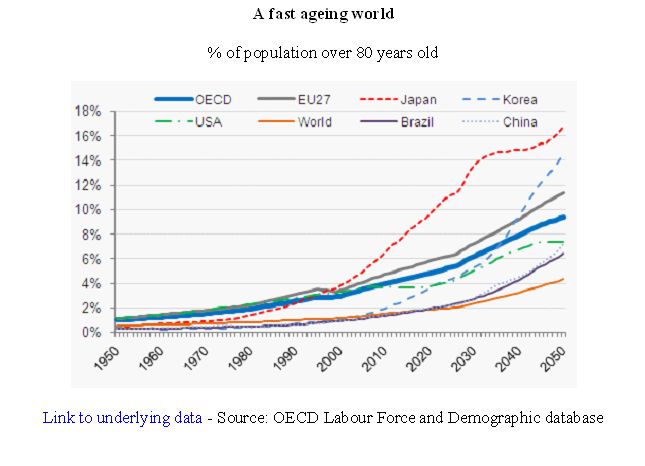
“Help Wanted? Providing and paying for long-term care” says that half of all people who need long-term care are over 80 years old. And the share of the population in this age group in OECD countries will reach nearly one in ten by 2050, up sharply from one in 25 in 2010. This percentage will reach 17% in Japan and 15% in Germany by 2050.
Spending on long-term care, which now accounts for 1.5% of GDP on average across the OECD, will rise accordingly. Sweden and the Netherlands today spend the most, at 3.5% and 3.6% respectively of GDP, while Portugal (0.1%), the Czech Republic (0.2%) and the Slovak Republic (0.2%) spend the least.
“With costs rising fast, countries must get better value for money from their spending on long-term care,” said OECD Secretary-General Angel Gurría. “The piecemeal policies in place in many countries must be overhauled in order to boost productivity and support family carers who are the backbone of long-term care systems.”
Major reforms to attract more care workers and retain them in the sector should be put in place quickly. Most long-term care careers are dead-end jobs with a high turnover and low pay and benefits, says the OECD. And caring for others comes at a price: caregivers are less likely to have a job than the average person and, if they do, it’s more likely to be part-time with fewer hours. They also face an increased risk of poverty and are more likely to suffer from mental health problems.
Upgrading the status of the long-term care workforce by improving pay and working conditions is key. Germany, the Netherlands, Sweden and Norway have boosted retention through recent initiatives along these lines. In Belgium, the Netherlands and Sweden, collective labour agreements that recognise years of experience in wage levels have also proved effective.
To meet future demand, countries will also need to attract more migrants who already make up a substantial part of long-term care workers in many OECD countries: from around one in four in Australia, the UK and the US, for example, to one in two in Austria, Greece, Israel and Italy.
In many countries, migrants are paid less than native-born workers, despite often being more qualified. One proposal would be to extend work permits to care workers in immigration quotas, as happens in Australia and Canada. Offering education and training, especially language skills, would also help.
Governments will need to find a balance between offering access to good-quality care and making their systems financially sustainable, the report says. Around 70% of long-term care users receive services at home, but spending in institutional care accounts for 62% of total spending. Respite care, encouraging part-time work and paying benefits to family carers can all be cost-effective policies, reducing demand for expensive institutional care.
Long-term care is too expensive for all but the richest to afford. Even people with above- average incomes could end up spending 60% of their disposable income on care costs. Countries have to spread the burden of such high costs, either by targeting universal benefits to those most in need of care or via public-private partnerships.
Private insurance could play a role in some countries, the report notes, but is likely to remain a niche market unless made compulsory. In the US and France, the largest such markets in the OECD, 5% and 15% respectively of people aged over 40 have a long-term care policy.
A country profile of long-term care in Ireland forms part of this study can be downloaded below